We all know that there is a risk of breast cancer that comes with the fact of being born female. And the way to find breast cancer early is this thing called the mammogram. Maybe you just had your first mammogram and received a call that you need to return for further imaging – how concerned should you be? Maybe you have had annual mammograms for 10 years and still wonder what it means that your breasts are apparently “heterogeneously dense.” Let’s review the mammogram technology and what these specialized x-rays mean for you and your breasts.
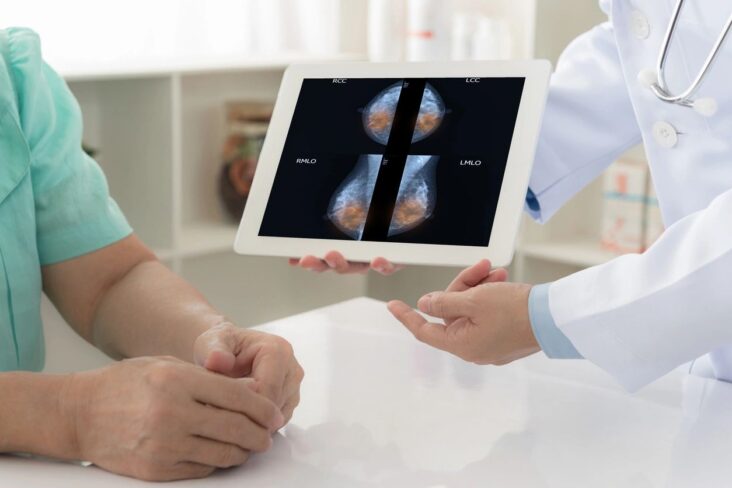
Mammograms, like all x-rays, use ionizing radiation to create images of your breast tissue. The breast is compressed between 2 paddles and multiple angles of x-rays are applied to create either a 2D or 3D image. Though unpleasant, the compression improves the quality of the image for the interpreting radiologist, helps keep the breasts steady to avoid artifact, and limits the radiation exposure by minimizing the volume of imaged tissue. The x-rays for mammograms are lower energy than that needed for imaging bones. Though excess radiation is something we know to avoid generally, the amount of radiation from a routine mammogram is 0.4milisieverts, roughly equivalent to the amount of background radiation (the amount our body is exposed to by the earth, water, stars, man-made things, etc) we are exposed to over about 8 weeks, so a mammogram is considered quite safe particularly when weighed against the risk of missing an early breast cancer.
There are 2 primary types of mammograms: screening and diagnostic. Screening mammograms are for the annual check of the entire breasts when there is no particular concern. Diagnostic mammograms focus on a specific area of concern and employ additional x-ray views for assessment of the area; they take a little longer and the radiologist is usually reviewing the images while you are still there in case further evaluation is needed.
The risk of breast cancer increases with age. The guidelines of when to have your first screening mammogram have been determined based on weighing the drawbacks of the mammogram with its benefits. The drawbacks include the time and expense of the test, a chance of a false positive results (with its unnecessary anxiety and further testing), and the minimal radiation exposure. The benefit is finding breast cancer and therefore easier or more successful treatment and survival. According to the American Cancer Society and the American College of Obstetricians and Gynecologists, age 40 is when the benefit outweighs the drawbacks for most women. Those with a with a history of breast issues or a family history of breast cancer may be an exception and should discuss breast cancer screening with your healthcare provider individually.
Mammograms are certainly not perfect. As mentioned previously, there are false positive results, meaning an abnormal finding that is actually benign after further imaging or a biopsy. Younger women and women with more dense breasts are more likely to have false positives. If you get a call requiring additional imaging, remember than most women who get a call back for further imaging do not have cancer. Additionally, the false negative rate, meaning that cancer is there and the mammogram misses it, is estimated at about 10%. For woman with dense breasts, 3D imaging with tomosynthesis can be used to increase accuracy. Ultrasound is another modality which may be recommended by the radiologist after the mammogram, particularly when evaluating an area of concern. Ultrasound is also useful for imaging the breasts of younger women.
The birads scoring system is something used by radiologists which helps to standardize results. The following is a summary of what each birads category means:
Birads 0: Need additional imaging or prior imaging records to complete evaluation
Birads 1: Negative — no action other than 12 month follow-up
Birads 2: Benign — breast findings which are stable and/or confidently benign, no action other than 12 month follow-up
Birads 3: Probably benign — short interval follow-up, typically 6 months
Birads 4: Suspicious — requires a tissue diagnosis (biopsy)
Birads 5: Highly suggestive of malignancy — more than 95% likely is cancer, requires a tissue diagnosis (biopsy)
Birads 6: Known malignancy, already biopsy-proven — monitoring progression or treatment response
In the common event of a birads 0, you will be called back usually for additional x-rays or an ultrasound. This is common if it is your first mammogram because there is less certainty about your breasts before there are multiple years worth of images to compare. Sometimes with a birads 0, they will simply need to obtain and review previous mammograms if you have had them. The call back experience may make you nervous, but reassuringly, 9 times out of 10 the final results are benign.
In addition to the birads category, you will usually see a breast density description on your mammogram report. It is determined as 1 of 4 levels: almost entirely fatty, scattered areas of fibroglandular density, heterogeneously dense, or extremely dense. The majority of women will be one of the middle two categories. The breast density can only be determined through mammography (you can’t tell just by feeling or examining your breasts). People with breasts rated as heterogeneously or extremely dense have a higher risk of breast cancer. Part of this is because the dense areas can “hide” an early mass, but even aside from this, it is thought that dense breasts in themselves bear a higher lifetime risk of cancer. If you have other increased risks for breast cancer along with dense breasts, you may be a candidate to have breast MRIs annually in addition to mammograms — a topic for another article, but please discuss with us in the office if you wonder about this for yourself.
Lastly, a word about the time-honored self breast exams: they are a worthwhile detection method, however, they are limited and very non-specific and if any lump or new mass is felt, diagnostic imaging is additionally necessary. And just because you don’t feel a new lump or mass, it doesn’t mean that there aren’t abnormalities which are small, deep in the tissue, or simply non-palpable. This is why mammograms, friends. It is not recommended to rely on self breast exams alone as a cancer screening method.
So mammograms, like humans, are flawed but incredibly valuable things. Thanks for reading and let’s talk about what’s right for your breasts at your next annual visit.